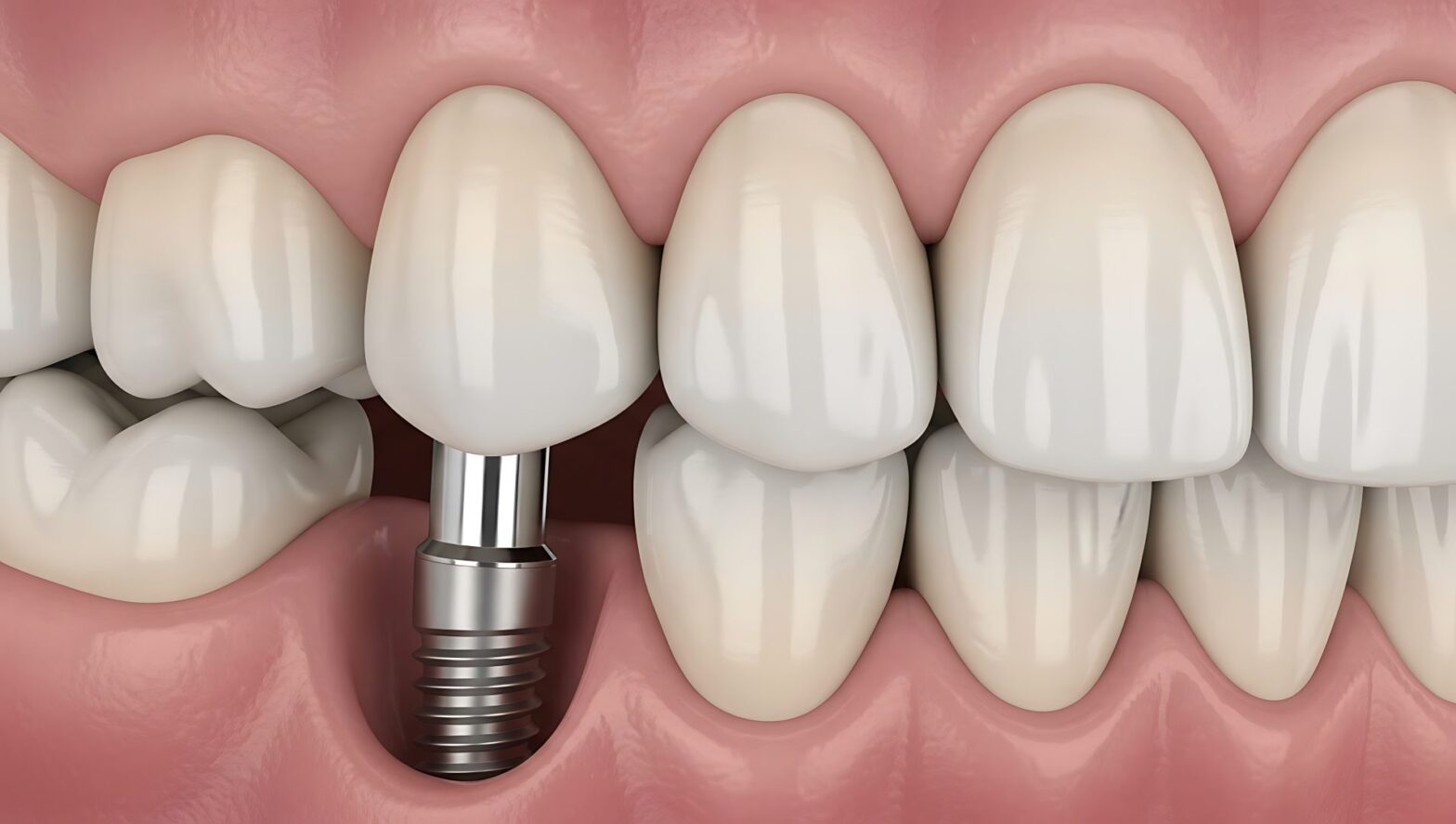
Successful dental implant therapy is fundamentally dependent on adequate bone volume and quality. In patients with alveolar bone loss due to periodontal disease, trauma, or long-term edentulism, insufficient bone remains a primary limiting factor for predictable implant placement.
As a result, recent research has increasingly focused on improving bone regeneration techniques to enhance implant stability and long-term outcomes.
Guided bone regeneration (GBR) remains a widely used approach in clinical practice. The technique involves the use of barrier membranes in combination with bone graft materials to facilitate new bone formation while preventing soft tissue ingrowth.
Advances in biomaterials, including xenografts, allografts, and synthetic substitutes, have improved handling characteristics and osteoconductive potential. More recently, bioactive materials incorporating growth factors and signaling molecules have shown promise in accelerating the regenerative process.
Platelet-rich fibrin (PRF) has also gained attention as an adjunctive therapy. Derived from autologous blood, PRF contains a high concentration of platelets, leukocytes, and cytokines that contribute to wound healing and angiogenesis. Clinical studies suggest that PRF may improve soft tissue healing and support early bone formation when used alongside grafting procedures.
Primary implant stability remains a critical determinant of osseointegration. Factors such as bone density, implant design, and surgical technique all play a role in achieving adequate stability at placement. In recent years, modifications in implant surface technology, including micro- and nano-texturing, have been introduced to enhance bone-to-implant contact and improve integration rates, particularly in compromised bone conditions.
“In implant dentistry, achieving and maintaining stability is directly linked to the quality of the surrounding bone and the body’s ability to regenerate tissue effectively,” says Dr. Arash Ravanbakhsh. “Advances in bone grafting materials and biologic adjuncts are allowing us to treat more complex cases with greater predictability and improved long-term outcomes.”
Immediate and early loading protocols have also been influenced by these advancements. With improved implant design and enhanced regenerative techniques, clinicians are increasingly able to reduce healing times while maintaining high success rates. However, careful case selection remains essential, particularly in patients with systemic risk factors such as smoking or uncontrolled diabetes.
From a clinical standpoint, the integration of regenerative techniques into implant workflows requires a comprehensive understanding of both surgical principles and material science. Proper case planning, including radiographic evaluation and assessment of bone morphology, is essential in determining whether augmentation procedures are required prior to or at the time of implant placement.
As research continues to evolve, the focus in implant dentistry is shifting toward biologically driven solutions that enhance the body’s natural regenerative capacity. These approaches not only expand the pool of patients eligible for implant treatment but also contribute to more stable and durable outcomes over time.